[tsf_breadcrumb sep="/" class="breadcrumbs]
Home / Patients / Specialty Services / Total Hip Replacement
Total hip replacement (THR) surgery can significantly reduce pain and improve mobility–but achieving the best possible outcome depends heavily on the rehabilitation process that follows. This webpage provides a comprehensive guide to the essential role of physical therapy (PT) in recovery after a total hip replacement, outlining how targeted rehabilitation supports healing, restores strength and mobility, and promotes long-term joint function.
Designed for individuals who have undergone hip replacement surgery, those preparing for the procedure, and caregivers supporting a loved one through recovery, this resource explains what to expect from PT at every stage. From early mobility and pain management to strength building and return to daily activities, PT serves as a critical component in helping patients regain independence and confidently return to an active lifestyle.
PT for total hip replacement is a specialized rehabilitation process designed to help patients regain strength, mobility, and function both before and after hip replacement surgery. It involves guided exercises, movement retraining, and activity progression aimed at restoring joint mobility, improving muscle strength, and promoting safe, independent movement throughout recovery.
Total hip replacement is one of the most commonly performed elective orthopedic surgeries worldwide, with over one million procedures performed annually, primarily to relieve pain and improve function in patients with end-stage hip osteoarthritis–most often affecting older adults, with a median age around the late 60s and a balanced mix of male and female patients undergoing surgery.1
PT begins with a thorough preoperative assessment to evaluate baseline strength, mobility, and functional status, which may help inform individualized goals and prepare the body for surgery. Postoperatively, structured PT is essential to reduce pain, restore range of motion (ROM), promote strength gains, and optimize functional outcomes throughout recovery, Research shows that patients who participate in consistent pre-and postoperative rehabilitation often experience enhanced physical function and a more confident return to everyday activities compared to less structured approaches.2
A total hip replacement is most commonly performed to relieve chronic pain and restore function when conservative treatments are no longer effective. The leading cause is osteoarthritis, a degenerative joint disease that results in progressive cartilage breakdown, joint stiffness, inflammation, and pain that limits mobility and daily activities.3 As cartilage wears away bone-on-bone contact can significantly impair walking, standing, and overall quality of life.
Hip fractures, particularly in older adults, are another major reason for hip replacement. When fractures are severe or the blood supply to the femoral head is compromised, total hip replacement may be recommended to restore mobility and reduce complications associated with prolonged immobility.4
Developmental dysplasia of the hip (DDH) can also lead to early joint degeneration. In this condition, the hip joint does not form properly, resulting in abnormal joint mechanics that increase wear over time and may eventually require surgical intervention.5
Additionally, patients who have undergone prior hip surgeries or internal fixation for fractures may require total hip replacement if hardware fails, arthritis develops, or joint damage progresses. Failed previous procedures can lead to persistent pain, instability, or loss of function, making joint replacement a more durable long-term solution.6
Preparing for and recovering from a total hip replacement requires a structured and proactive approach. PT plays an essential role both before and after surgery, helping patients build strength, protect the joint, and support long-term function.
Engaging in preoperative PT can improve postoperative outcomes by strengthening the muscles surrounding the hip, improving mobility, and preparing patients for the demands of recovery. Preoperative exercise has been associated with improved early functional performance and greater confidence during the recovery process.2
Common pre-surgery exercises may include:
These exercises help optimize muscle activation and joint support prior to surgery, creating a stronger foundation for postoperative rehabilitation.
PT typically begins shortly after surgery, often within the first 24 hours, depending on medical status and surgical protocol. Early therapy focuses on safe mobility, proper use of assistive devices, restoring basic hip movement, and preventing complications such as stiffness or blood clots. Pain and swelling are addressed through guided movement, therapeutic exercise, positioning strategies, and gradual activity progression, Evidence supports early, structured rehabilitation to improve mobility and functional outcomes following a total hip replacement.7
Because every patient’s health status, surgical approach, and goals differ, a personalized treatment plan is essential. Physical therapists (PTs) assess strength, balance, gait mechanics, and functional needs to tailor rehabilitation appropriately. Seeking professional guidance ensures safe progression, reduces the risk of complications, and promotes a confident return to daily activities.
PT is a cornerstone of recovery after total hip replacement, guiding patients through a structured rehabilitation process designed to restore mobility, rebuild strength, improve balance, and promote long-term joint function. Rather than simply focusing on healing the surgical site, PT addresses the surrounding muscles, movement patterns, and functional activities that allow patients to return safely to daily life. Research supports structured postoperative rehabilitation to improve mobility, physical function, and overall recovery outcomes following total hip replacement surgery.7
Recovery begins with a comprehensive initial evaluation conducted by a licensed PT. This assessment includes measurement of hip ROM, muscle strength, gait mechanics, balance, pain levels, swelling, and functional mobility such as transfers, stair navigation, and walking tolerance. Understanding each patient’s baseline allows the PT to establish realistic goals and create a personalized plan of care that aligns with surgical precautions and individual recovery timelines.
At Confluent Health, the rehabilitation approach emphasizes individualized care, progressive exercise prescription, movement retraining, and patient education. Treatment plans are tailored to each patient’s surgical approach, medical history, activity level, and long-term goals. Through guided progression–beginning with early mobility and advancing to strengthening, balance training, and functional–PT supports safe recovery while helping patients regain confidence and independence.
By combining evidence-based rehabilitation with personalized guidance, PT plays a vital role in maximizing outcomes and helping patients return to meaningful activities after total hip replacement surgery.
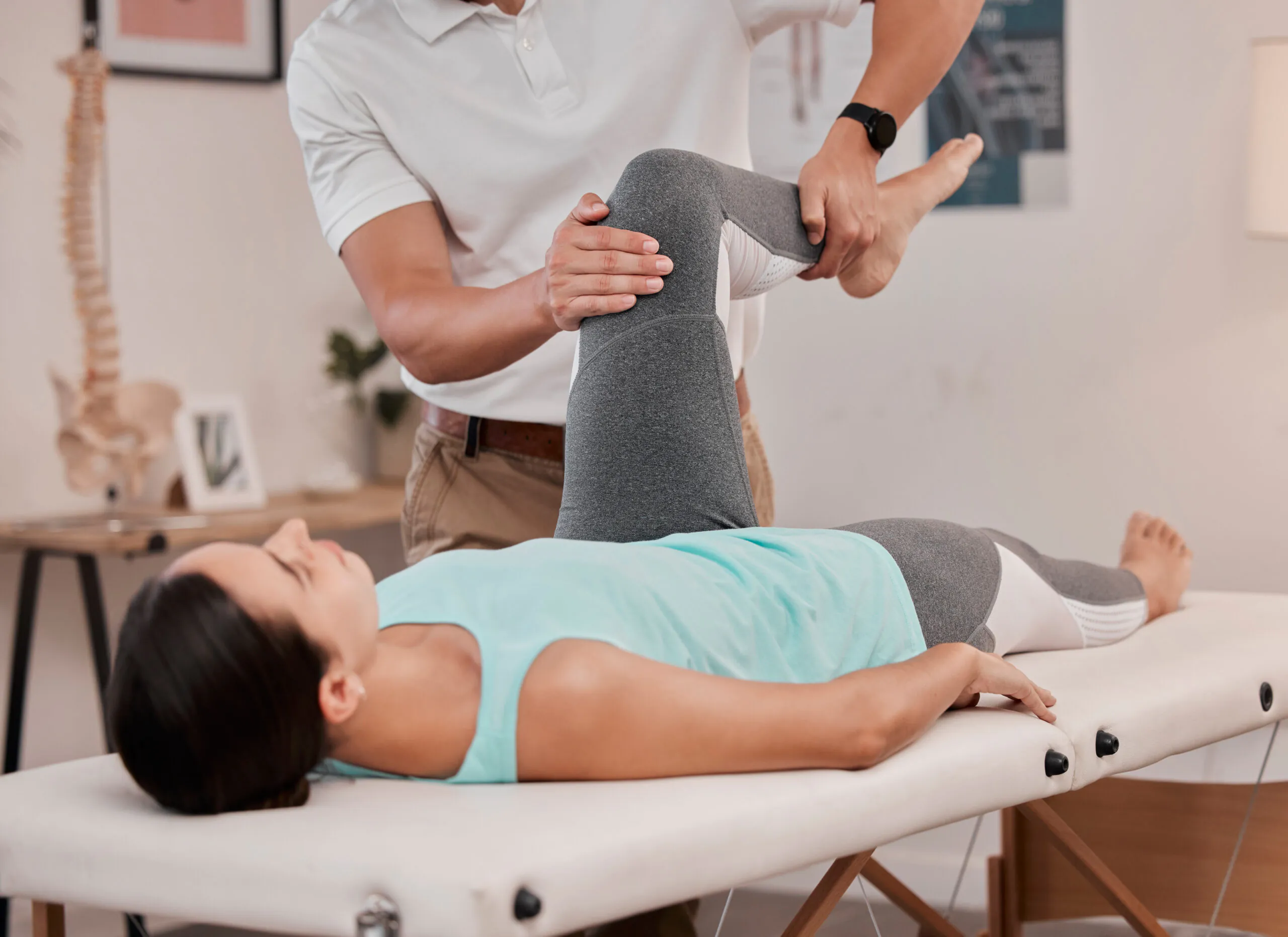
Restoring hip mobility is one of the earliest priorities after a total hip replacement. Regaining safe ROM helps normalized walking mechanics, improve comfort with daily activities, and reduce compensatory movement patterns. Early structured rehabilitation has been shown to improve functional mobility outcomes after a hip replacement.7
PTs introduce gentle, targeted exercises to improve hip joint mobility while respecting surgical precautions, these may include heel slides, assisted hip abduction, seated marches, and controlled hip extension movements. As healing progresses, flexibility exercises for the hip flexors, hamstrings, and surrounding musculature are gradually incorporated to improve overall movement efficiency and reduce stiffness.8
Guided progression is essential. PTs monitor swelling, pain levels, and movement quality to safely advance mobility exercises while protecting the surgical joint.
Once foundational mobility is established, rehabilitation shifts toward strengthening the muscles that support and stabilize the hip joint. Key muscle groups include the gluteus maximus, gluteus medius, hip flexors, quadriceps, and core musculature. Strengthening these muscles improves gait mechanics, reduces joint stress, and supports long-term functional outcomes.
Early strengthening exercises may include glute bridges, standing hip abduction, mini squats, and controlled step training. As strength improves, therapy progresses to more functional and resistance-based exercises that simulate real-life activity such as stair climbing, prolonged walking, and transitional movements.
A progressive strengthening plan is individualized based on healing stage, tolerance, and functional goals. Gradual increases in resistance, repetitions, and complexity ensure safe advancement while minimizing risk of overuse or setbacks.
Balance and stability are critical after total hip replacement, as surgery and temporary muscle weakness can affect proprioception and coordination. Targeted balance training has been shown to improve functional recovery and reduce call risk following joint replacement surgery.7
PTs incorporate progressive balance exercises such as weight shifting, single-leg stance (when appropriate), tandem walking, and dynamic gait activities. These interventions help retrain neuromuscular control and improve confidence during movement.
By emphasizing balance and stability alongside mobility and strength, PT helps reduce the risk of falls and postoperative complications. This comprehensive, individualized approach supports safer movement, improved independence, and long-term joint protection after total hip replacement surgery.

Pain management is an important component of recovery after a total hip replacement, particularly in the early stages of rehabilitation, PT focuses not only on reducing discomfort but also on addressing the underlying contributors to pain–such as swelling, stiffness, muscle weakness, and altered movement mechanics. A structured postoperative rehabilitation has been shown to improve pain levels and functional outcomes following total hip replacement.
PTs use a variety of non-pharmocological pain relief strategies during the rehabilitation process. These may include guided therapeutic exercise, manual therapy techniques, movement retrainting, swelling management strategies, positioning education, and activity pacing. Exercise-based rehabilitation is supported in the literature as an effective way to reduce postoperative pain while restoring mobility and strength.4
A personalized treatment plan is essential, as recovery experiences vary depending on surgical approach, health status, and activity goals. The patient-therapist partnership plays a critical role in successful recovery: open communications, shared goal-setting, and consistent participation help optimize outcomes. Patients experiencing ongoing discomfort are encouraged to take proactive steps and seek professional PT guidance to safely manage pain and support long-term recovery.
If you’ve undergone a total hip replacement–or are preparing for surgery–tailoring proactive steps with PT can significantly influence your recovery and long-term outcomes. Early, guided rehabilitation helps restore mobility, rebuild strength, improve balance, and manage pain in a safe and structured way. Booking a consultation with Confluent Health allows our experienced PTs to assess your individual needs and design a personalized plan tailored to your goals. Don’t wait to address concerns or lingering discomfort–schedule your appointment today and take an active role in your recovery.
PT plays a vital role in maximizing recovery after total hip replacement, supporting patients as they regain movement, strength, stability, and confidence. A personalized rehabilitation plan ensures that care is aligned with your specific health status, surgical approach, and long-term activity goals. Seeking professional guidance from a licensed PT helps optimize healing, reduce complications, and promote a safe return to daily life.
PT typically begins within 24 hours after surgery, depending on your surgeon’s protocol and medical status. However, you will be assessed by a PT within the hospital prior to discharge to ensure safe return to home. Early therapy focuses on safe mobility, walking with an assistive device, and gentle ROM exercises to prevent stiffness and promote circulation. Starting PT early helps support faster functional recovery and reduces the risk of complications.
Most patients participate in formal PT for approximately 6-12 weeks, though timelines vary based on age, overall health, and activity goals. Individuals are encouraged to continue strengthening and mobility exercises independently after discharge from supervised care. Your PT will adjust the plan based on your progress and functional needs.
Early exercises focus on restoring hip mobility and activating key muscle groups such as the glutes and hip stabilizers. As healing progresses, therapy advances to strengthening, balance training, and functional movements like stair climbing and prolonged walking. Exercises are tailored to your surgical precautions and long-term mobility goals.