[tsf_breadcrumb sep="/" class="breadcrumbs]
Home / Patients / Specialty Services / Shoulder Surgery
Recovering from shoulder surgery can feel overwhelming, but the right rehabilitation plan can make a significant difference in how quickly and safely you return to your normal activities. This guide is designed to provide a comprehensive overview of the role of physical therapy (PT) in post-operative shoulder recovery. Through targeted treatment strategies, PT helps reduce pain, restore mobility, rebuild strength, and improve overall function–ultimately enhancing quality of life after surgery.
Whether you have recently undergone a procedure or are preparing for one, understanding the rehabilitation process is essential. PT offers a structured, evidence-based approach that supports healing while minimizing complications and promoting long-term success. From early protection and mobility work to progressive strengthening and return-to-activity training, each phase of care is tailored to your specific procedure and goals.
This resource is intended for individuals recovering from shoulder surgery, patients preparing for an upcoming procedure, and healthcare professionals seeking to better understand the value of post-operative PT. By providing clear, practical information, it aims to empower patients to take an active role in their recovery and seek the professional guidance needed for optimal outcomes.
Post-shoulder surgery PT is a structured rehabilitation process designed to support healing, restore movement, and rebuild strength following a surgical procedure on the shoulder joint. This type of therapy is typically performed in phases, beginning with protection and gentle mobility and progressing to strengthening and functional retraining based on surgical precautions and tissue healing timelines. Research shows that guided rehabilitation is critical for optimizing surgical outcomes, reducing complications such as stiffness, and improving long-term shoulder function.1
The impact of post-operative shoulder rehabilitation on daily life is substantial. Without appropriate therapy, individuals may experience ongoing pain, reduced range of motion (ROM), and difficulty performing routine tasks such as dressing, reaching overhead, or lifting objects. Structured PT helps restore independence, improve confidence in movement, and facilitate a safe return to work, exercise, and daily activities.2
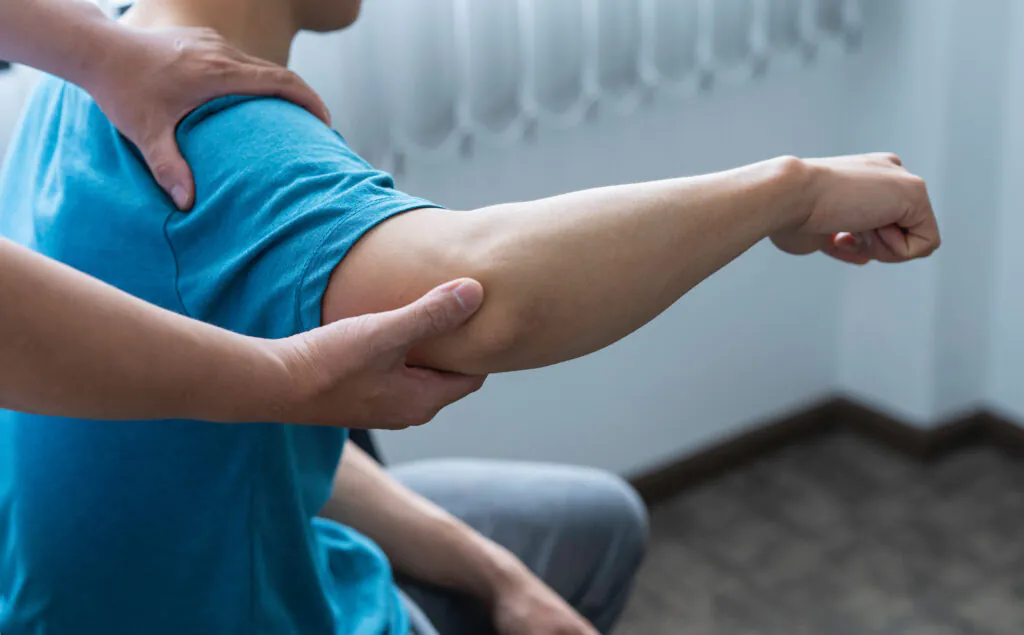
Shoulder surgeries are commonly performed to address pain, instability, or structural damage that does not improve with conservative care. Most modern procedures are performed arthroscopically, allowing for smaller incisions and typically faster recovery. Common surgeries include rotator cuff repair, labral repair, and proximal biceps tendon procedures such as tenodesis or tenotomy, as well as debridement to remove damaged tissue. In more advanced cases, such as severe joint degeneration, shoulder replacement surgery may be indicated.3
Post-operative rehabilitation is a critical component of recovery following these procedures. Without appropriate guidance, patients are at risk for complications including joint stiffness, persistent weakness, and reduced functional outcomes. PT ensures that healing tissues are protected while gradually reintroducing movement and load in a safe and effective manner.4
PT can address many common post-operative shoulder issues including pain, swelling, limited mobility, muscle weakness, scar tissue restrictions, and difficulty performing functional movements like reaching or lifting. Additionally, therapy focuses on restoring proper movement mechanics and joint stability, which are essential for long-term recovery and prevention of reinjury.2
The evaluation process for post-operative shoulder pain begins with a comprehensive assessment by a PT, focused on understanding the specific procedure performed, current symptoms, and stage of healing. Rather than relying on additional diagnostic imaging, therapists typically review the surgical report (operative note) and, when needed, communicate directly with the surgical team to ensure rehabilitation aligns with post-operative precautions and tissue healing timelines. This collaborative, informed approach helps guide safe and effective treatment progression.
Physical therapists (PTs) assess post-surgical pain and function through a combination of clinical measures, including observation of movement, ROM testing, strength assessment, and evaluation of functional tasks such as reaching or lifting. They also monitor pain levels, joint stiffness, swelling, and compensatory movement patterns that may develop during recovery. These findings help identify limitations and guide appropriate progression of mobility and strengthening interventions.1
Personalization is a critical component of post-operative shoulder rehabilitation. Not all surgeries–or patients–are the same. For example, a massive rotator cuff repair requires a significantly different timeline and loading strategy as compared to a smaller repair or simple debridement. Factors such as age, tissue quality, overall health, and activity goals all influence the rehabilitation plan. Because of this variability, a one-size-fits-all approach is not appropriate, and individualized care is essential for optimal recovery. 4
Living with post-operative shoulder pain can be challenging, particularly in the early stages of recovery when movement is limited and discomfort is more pronounced. Effective coping strategies include adhering to activity guidelines, gradually progressing movement as tolerated, using prescribed exercises to maintain mobility, and modifying daily tasks to reduce strain on the healing shoulder. Education on pain expectations and pacing activity is also key to avoiding setbacks during recovery.2
A personalized rehabilitation plan remains essential throughout the recovery process. Individual differences in surgical procedure, healing rate, and functional goals require a tailored approach to ensure safe progression and optimal outcomes. Working closely with a PT allows for adjustments based on symptoms, helping to manage flare-ups while continuing to build strength and mobility over time.
Seeking professional guidance and support can make a significant difference in both physical and emotional recovery. Post-surgical pain and temporary limitations can impact mental well-being, making reassurance, education, and structured progression especially important. With the right support and a well-designed plan, patients can successfully navigate recovery, regain confidence in movement, and promote long-term shoulder health and function.
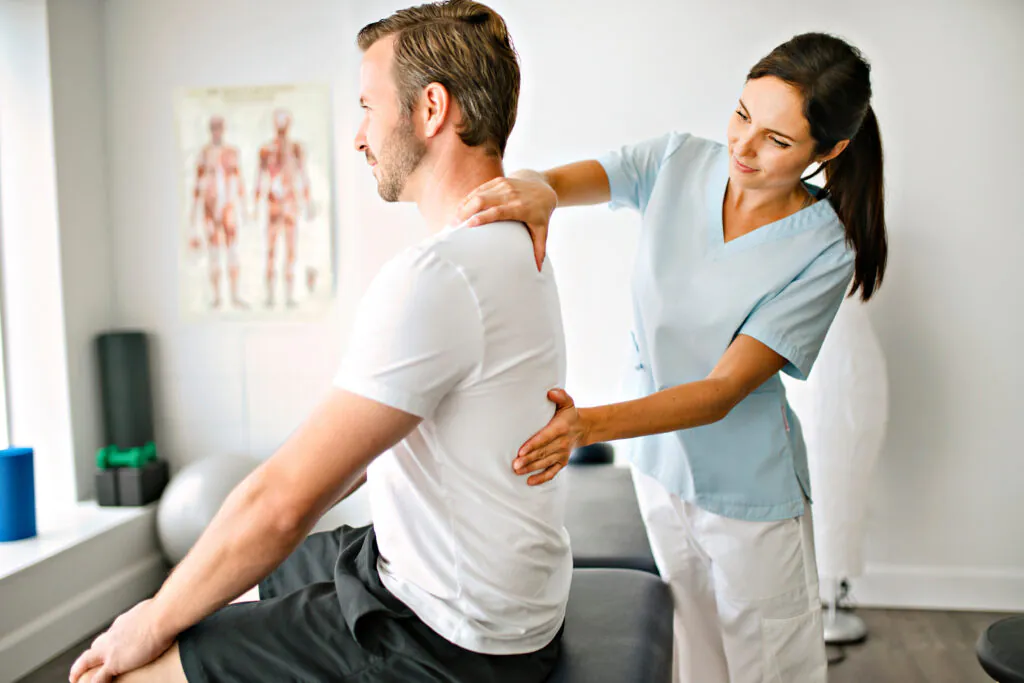
Post-surgical PT for shoulder procedures offers significant benefits in both the short and long term. Patients who engage in structured rehabilitation programs often experience reduced pain, improved ROM, increased strength, and faster return to daily activities and work tasks as compared to those who do not receive guided therapy.4 Consistent therapy also helps prevent complications such as stiffness, loss of function, and compensatory movement patterns that can lead to secondary injuries.
Many patients report tangible improvements in their quality of life after completing post-operative PT. For example, individuals recovering from rotator cuff repair often regain the ability to lift overhead, perform household tasks, and return to recreational activities such as swimming or tennis with greater confidence. Personalized guidance from a PT ensures that exercises are performed safely and effectively, promoting both healing and long-term joint health. Patient testimonials frequently highlight the reassurance, motivation, and structured progression provided by therapy, which contributes to both physical and psychological recovery.1
Recovery from shoulder surgery is a gradual process, and the timeline depends on the type of procedure, the severity of the injury, and individual factors such as age, overall health, and adherence to rehabilitation. While each patient’s journey is unique, post-operative recovery generally follows a phased approach that balances protection of healing tissues with progressive restoration of movement, strength, and function.4
During the first few weeks after surgery, the primary goals are to protect the repair, control pain and inflammation, and maintain gentle mobility in non-involved joints. The shoulder may be immobilized in a sling or brace depending on the procedure. PT at this stage focuses on patient education, gentle pendulum exercises, and passive or assisted ROM exercises within safe limits. Patients are encouraged to avoid lifting, pushing, or pulling to protect the surgical repair.
As healing progresses, patients begin more active ROM exercises under the guidance of a PT. These exercises help restore flexibility, reduce stiffness, and promote circulation without stressing the repaired tissues. Light functional activities may be introduced, and PTs often monitor for compensatory movements to prevent secondary issues. Pain should gradually decrease, and patients typically start regaining confidence in shoulder movement.1,4
Once adequate healing and mobility are achieved, progressive strengthening exercises are introduced. This includes targeted rotator cuff and scapular stabilizer strengthening, resistance training, and functional movement patterns. Therapy focuses on rebuilding muscle endurance, coordination, and stability needed for everyday tasks. Patients may begin more dynamic activities under supervision while continuing to avoid high-risk movements or heavy lifting.1,4
The final phase involves advanced strengthening, sport-specific training, and functional activity reintegration. Patients may gradually return to work, recreational sports, or higher-demand physical activities. Full recovery can take anywhere from three to six months for most arthroscopic procedures while more extensive surgeries, such as a shoulder replacement or massive rotator cuff repair, may require six months to a year for complete functional recovery.1,4
Setting realistic expectations is essential. Progress is rarely linear, and flare-ups or temporary setbacks can occur. Consistent adherence to a structured individualized PT plan is the most reliable way to achieve optimal outcomes, restore function, and reduce the risk of reinjury.

Preventing future shoulder issues after surgery requires a proactive and consistent approach to maintaining mobility, strength, and overall shoulder health. One of the most important factors is engaging in PT early in the recovery process, particularly to restore safe ROM while respecting healing timelines. Early, guided mobility has been shown to reduce the risk of post-operative stiffness and improve long-term functional outcomes when appropriately progressed.4
Long-term prevention also depends on maintaining adequate strength and stability of the shoulder complex. This includes not only the rotator cuff muscles, but also the surrounding scapular stabilizers that help support proper shoulder mechanics. Ongoing participation in a structured exercise program–even after formal therapy has ended–can help preserve these gains and reduce the likelihood of reinjury or chronic dysfunction.1
Additionally, addressing movement patterns, posture, and activity habits plays a key role in preventing recurrence. Gradually returning to higher-level activities, avoiding sudden increases in load or intensity, and incorporating regular mobility work can help the shoulder adapt safely over time. Seeking guidance from a PT early–whether for post-operative care or at the first sign of recurring symptoms-can help identify potential issues before they progress.
By prioritizing early rehabilitation, maintaining strength and flexibility, and staying mindful of activity progression, individuals can support long-term shoulder health, improve resilience, and reduce the risk of future injury.
Recovering from shoulder surgery is a process–and you don’t have to navigate it alone. Taking a proactive approach by starting post-surgical PT early can help reduce pain, restore mobility, and ensure you regain strength safely and effectively. Delaying care or trying to manage recovery on your own can lead to stiffness, prolonged discomfort, or setbacks that slow your progress.
Choosing the right PT is an important part of your recovery. Look for a provider who has experience with post-operative shoulder rehabilitation, communicates clearly, and develops individualized treatment plans based on your specific procedure and goals. A strong patient-therapist partnership is essential-your therapist should not only guide your exercises but also educate and support you throughout each phase of recovery, helping you feel confident in your progress.
Working with a trusted provider like Confluent Health ensures you receive evidence-based care tailored to your needs. Their team emphasizes collaboration, personalized treatment ,and long-term success–helpng you return to daily activities, work, and recreation with confidence.
If you’ve recently had shoulder surgery or are preparing for one, now is the time to take the next step. Schedule a consultation with a PT at Confluent Health to begin a structured, individualized recovery plan and set yourself up for the best possible outcome.
Home exercises are typically performed daily, though the exact frequency and intensity depend on your stage of recovery and the type of surgery you had. Early on, this may involve gentle ROM exercises multiple times per day, while later phases focus on strengthening a few times per week. It’s important to follow your PTs specific recommendations to ensure safe and effective progression as the HEP is designed to meet your individual goals while maintaining surgical precautions.
The timeline for discontinuing a sling varies based on the procedure and surgeon protocol, but it’s commonly worn for about 2-6 weeks after surgery. More extensive repairs, such as rotator cuff repairs, often require longer immobilization compared to simpler procedures. Always follow guidance from your surgeon and PT, as removing the sling too early can compromise healing.