[tsf_breadcrumb sep="/" class="breadcrumbs]
Home / Patients / Specialty Services / Lymphedema
Lymphedema is a chronic condition that can cause swelling, discomfort, reduced mobility, and changes in daily function. While it often requires long-term management, physical therapy (PT) plays a critical role in helping individuals control symptoms, reduce pain, and improve overall quality of life. With the right combination of specialized techniques, therapeutic exercise, and patient education many people with lymphedema can successfully manage their condition and return to meaningful daily activities.
This guide is designed to provide a comprehensive overview of how PT supports the treatment and recovery process for lymphedema. It will explore the techniques and approaches used by trained therapists, the benefits of structured rehabilitation programs, and the importance of early, professional intervention. This resource aims to provide clear, practical, and evidence-based guidance to those living with lymphedema and seeking treatment options, those wanting to better understand how PT can help manage swelling and function, and referring healthcare professionals looking for insight into the benefits of rehabilitation services.
Lymphedema is a chronic condition in which lymphatic fluid fails to drain properly, causing persistent swelling often in the arms, legs, or trunk due to lymphatic system dysfunction or damage. It can be primary (from congenital or genetic abnormalities) or secondary (typically resulting from injury, surgery, infection, or cancer treatment) and leads to protein-rich fluid accumulation in the tissues. Accurate diagnosis and early management are crucial to prevent progression and complications such as recurrent infections, skin changes, and functional impairment.1
Prevalence estimates suggest that 3-5 million people in the United States live with lymphedema, though the true number may be higher due to underdiagnosis and underreporting of the condition.2 Worldwide, lymphedema is considered a major but underrecognized health challenge affecting tens to hundreds of millions of individuals.3 In cancer survivors, lymphedema is a common sequela of lymph node removal or radiation therapy; for example, estimates of breast cancer-related lymphedema range from about 6% to 30% depending on surgical and treatment factors.3
Studies show that lymphedema is more common in women than in men, although the exact difference varies depending on the type of lymphedema and population studied. For example, large data analyses indicate a higher estimated prevalence among women compared with men, suggesting up to roughly 1.8 times higher prevalence in females in that dataset.4
The swelling, heaviness, and limited range of motion (ROM) associated with lymphedema can significantly disrupt daily activities such as dressing, walking, or working, Physical discomfort, decreased limb function, and frequent episodes of cellulitis or skin breakdown contribute to physical limitations and may worsen psychological distress or reduce quality of life.1 Early engagement with PT and comprehensive management strategies can help mitigate these impacts and support long-term function.
Lymphedema develops when the lymphatic system – a network of vessels and nodes responsible for returning excess fluid from tissues back into circulation – cannot adequately transport lymph fluid, leading to persistent swelling and fluid buildup in the affected area (typically arms or legs). This condition falls into two broad categories based on its underlying cause: primary lymphedema and secondary lymphedema.1
Primary lymphedema arises from congenital or genetic abnormalities of the lymphatic system itself. These developmental defects may result in absent, underdeveloped, malformed, or improperly functioning lymphatic vessels, preventing normal fluid drainage. Primary lymphedema may be present at birth (congenital), emerge around puberty (praecox), or develop later in adulthood (tarda), depending on the specific cause and genetic background.3
In contrast, secondary lymphedema is caused by acquired damage, obstruction, or trauma to an otherwise normal lymphatic system. The most common causes include lymph node removal or radiation therapy during cancer treatment, which can disrupt or scar lymphatic pathways, impairing fluid flow.1 Other contributors may involve severe infections, traumatic injury, chronic inflammation, or parasitic infections such as filariasis in endemic regions, which block or injure lymphatic vessels.3
Understanding whether lymphedema is primary or secondary is critical for appropriate management, risk assessment, and individualized treatment planning. Early identification of the underlying cause helps guide interventions aimed at reducing swelling, maintaining function, and minimizing complications.

Lymphedema symptoms typically develop gradually and may worsen over time if not properly managed. The most common sign is persistent swelling, usually in one arm or leg, although it can occur in the chest wall, abdomen, neck, or genital region depending on the underlying cause. In early stages, swelling may fluctuate throughout the day, but it often becomes more constant as the condition progresses. 1
Individuals frequently report a feeling of heaviness, tightness, or fullness in the affected limb. As fluid accumulates, patients may experience restricted ROM, difficulty fitting into clothing or jewelry, and reduced functional use of the limb. Over time, chronic fluid buildup can lead to skin changes, including thickening, hardening (fibrosis), dryness, or recurrent infections such as cellulitis.5 Early recognition of these symptoms is important, as prompt intervention can help slow progression and reduce complications.

Lymphedema is often diagnosed clinically through a detailed medical history and physical examination. Individuals experiencing unexplained or persistent swelling–esepcially after cancer treatment, surgery, or infection–should consider consulting a physical therapist trained in lymphedema management, who can assess symptoms and determine whether further medical evaluation is warranted. Physical therapists (PTs) are trained to identify concerning signs and will refer to a physician when necessary for additional diagnostic workup.
Diagnostic testing may be recommended to confirm the diagnosis or rule out other causes of swelling. Imaging studies such as lymphoscintigraphy, ultrasound, MRI, or CT scans can help evaluate lymphatic function and exclude alternative conditions like deep vein thrombosis or tumors.1 In oncology-related cases, physicians may also review surgical history and prior radiation exposure when assessing risk.5
During a PT evaluation, therapists assess limb circumference or volume measurements, tissue texture, skin integrity, ROM, strength, and functional mobility. They may compare both limbs for asymmetry and evaluate for pitting edema or fibrotic tissue changes. This comprehensive assessment guides the development of an individualized treatment plan aimed at reducing swelling, improving mobility, and preventing progression.
Treatment for lymphedema focuses on reducing swelling, preventing complications, and improving overall limb function. In most cases, management begins with non-surgical (conservative) interventions, which are considered the standard of care and can significantly improve symptoms when performed consistently and correctly.
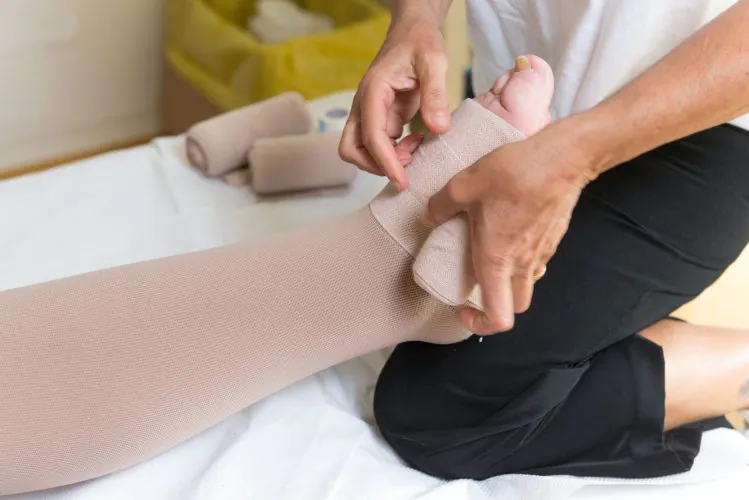
Compression Therapy is a cornerstone of lymphedema management. This may include multilayer compression bandaging during intensive treatment phases and the use of properly fitted compression garments for long-term maintenance. Compression helps move lymph fluid out of the affected limb and prevent reaccumulation.5
Manual lymphatic drainage (MLD) is a specialized, gentle hands-on technique performed by a trained PT to stimulate lymph flow and redirect fluid toward functioning lymphatic pathways. MLD is often combined with compression therapy as part of Complete Decongestive Therapy, a widely accepted treatment approach.1
Exercise plays a key role in promoting lymphatic circulation. Guided, low-intensity movements and progressive strengthening exercises help activate muscle pumps that assist lymph flow without overloading the limb. When appropriately prescribed, exercise is safe and beneficial for individuals with lymphedema.
Skin Care is essential to reduce infection risk. Keeping the skin clean, moisturized, and protected helps prevent breakdown and cellulitis, which can worsen swelling and damage lymphatic structures.1
In some cases, pneumatic compression pumps may be recommended. These devices use inflatable sleeves to apply intermittent pressure, assisting with fluid movement when combined with other therapies.5
Surgical interventions are generally considered when conservative management does not adequately control symptoms. The goal of surgery is to improve lymphatic drainage and reduce swelling by restoring or enhancing lymph flow pathways.
Common procedures include lymphatic bypass (lymphovenous anastomosis), which connects lymphatic vessels directly to nearby veins to improve fluid drainage, and vascularized lymph node transfer, in which healthy lymph nodes are transplanted to the affected area to promote new lymphatic function. These microsurgical techniques aim to reduce limb volume, improve symptoms, and decrease infection frequency in carefully selected patients.1
Treatment decisions are individualized based on severity, underlying cause, and patient goals. In most cases, PT remains the foundation of care, with surgery serving as an adjunct option for select individuals.
While not all cases of lymphedema can be prevented, certain strategies can significantly reduce the risk of developing or worsening the condition–particularly for individuals at higher risk following cancer treatment or lymph node removal. Preventative care focuses on protecting the lymphatic system, minimizing inflammation, and supporting overall health.
Protecting the skin from injury and infection is essential, as even minor cuts, burns, insect bits, or skin breakdown can trigger inflammation and increase lymphatic load. Proper hygiene, regular moisturizing, prompt treatment of wounds, and avoiding needle sticks or blood pressure measurements in at-risk limbs are commonly recommended precautions.5
Maintaining a healthy body weight is also important, as obesity has been identified as a risk factor for both the development and progression of lymphedema. Excess adipose tissue can impair lymphatic function and increase mechanical stress on the lymphatic system.1
Engaging in appropriate, supervised exercise can help stimulate lymphatic flow and maintain mobility. Gradual, progressive strength training and low-impact aerobic activity has been shown to be safe and beneficial when properly guided, helping reduce swelling risk and improve overall limb function.5
Lymphedema is a chronic condition that requires ongoing management, but with the right support, individuals can maintain an active and fulfilling lifestyle. Effective coping strategies include consistent use of compression garments (when prescribed), adherence to home exercise programs, skin care routines, and monitoring for early signs of increased swelling or infection. Education and self-management are central components of long-term success.1
During flare-ups, individuals may benefit from temporarily increasing compression, elevating the affected limb, performing gentle lymphatic exercises, and contacting their healthcare provider if signs of infection such as redness, warmth, or fever develop. Early response to symptom changes can help prevent progression.5
Because lymphedema varies in severity and presentation, a personalized treatment plan developed in collaboration with a PT or lymphedema specialist is essential. Individualized care ensures that compression levels, exercise intensity, and manual techniques are tailored to each patient’s needs, lifestyle, and goals. Ongoing professional guidance supports not only symptom control but also long-term function, independence, and overall well-being.
Seeking professional evaluation and consistent follow-up care empowers individuals to manage lymphedema proactively, reduce complications, and promote lifelong lymphatic health.
PT is a central component of lymphedema management, beginning with a thorough initial assessment. During the first visit, a PT reviews medical history, evaluates limb circumference or volume measurements assesses, skin integrity and tissue texture, and examines ROM, strength, posture, and functional mobility, This comprehensive evaluation helps determine the stage and severity of lymphedema and guides development of an individualized plan of care.
Treatment commonly includes elements of Complete Decongestive Therapy (CDT)–the gold standard conservative approach–which combines manual lymphatic drainage, compression bandaging or garment fitting, therapeutic exercise, and skin care education.1 Therapists may incorporate progressive strengthening, low-impact aerobic conditioning, diaphragmatic breathing, and mobility exercises to support lymph flow and improve overall function. Education is a critical component, empowering patients with self-management strategies, proper garment use, and early recognition of flare-ups.
The goals of PT include reducing limb volume, preventing progression, minimizing infection risk, restoring mobility, and improving participation in daily activities. Beyond swelling reduction, PT focuses on long-term independence and sustainable symptom control.
When selecting a provider, patients should look for a licensed PT with specialized training or certification in lymphedema management. Experience in compression therapy, MLD, and oncology rehabilitation is particularly important. A strong patient-therapist partnership–built on communication, shared goals, and consistent follow-up–plays a vital role in achieving successful outcomes.
Consistent participation in PT has been shown to significantly reduce limb swelling, improve ROM, decrease discomfort, and enhance overall quality of life.5 Many patients report improved ease with daily tasks, better tolerance for exercise, and increased confidence in managing their condition independently.
In addition to physical improvements, therapy can reduce the frequency of complications such as cellulitis and help prevent long-term tissue changes associated with chronic swelling.2 By combining clinical experience with individualized care, PT supports both immediate symptom relief and long-term lymphatic health.
Ultimately, PT offers more than symptom management–it provides patients with the tools, education, and support needed to live actively and confidently with lymphedema.
A typical session begins with a thorough assessment of limb volume, ROM, strength, and skin condition. Treatment often includes manual lymphatic drainage, compression bandaging or garment fitting, therapeutic exercises, and skin care education, all tailored to the patient’s specific needs and stage of lymphedema.
Results vary depending on the severity and duration of lymphedema, but many patients notice reduced swelling, improved mobility, and greater comfort within a few weeks of consistent therapy. Ongoing self-management and regular follow-ups are key to maintaining long-term benefits.
PT cannot cure lymphedema, as it is a chronic condition but it is highly effective at controlling symptoms, preventing progression, and improving quality of life. With a structured program, patients can cause significant reduction in swelling, better limb function, and fewer complications.