[tsf_breadcrumb sep="/" class="breadcrumbs]
Home / Patients / Specialty Services / Total Knee Replacement
Total knee replacement surgery is a proven solution for reducing pain and improving function for individuals with severe knee arthritis or joint damage. Physical therapy (PT) maximizes the benefits of surgery by helping patients restore strength, mobility, and range of motion (ROM) while improving overall function. This page emphasizes the importance of PT, exercise, and structured rehabilitation in supporting a safe and effective recovery after total knee replacement (TKR). Whether you have already undergone surgery, are preparing for an upcoming procedure, or are supporting a loved one through recovery, this resource provides clear guidance on how PT helps patients achieve the best possible outcomes.
PT for total knee replacement is a specialized rehabilitation process designed to help patients regain strength, mobility, and functional independence before and after knee replacement surgery. It includes exercises and guided movement retraining that target ROM, muscle strength, gait mechanics, and activities of daily living (ADLs) to support recovery and optimal surgical outcomes.
Total knee replacement is one of the most common orthopedic procedures performed today. In the United States, hundreds of thousands of TKRs are done each year, with projected growth as the population ages and demand for joint pain relief increases.1 Among U.S. adults aged 50 years and older, an estimated 4.2% currently live with a total knee replacement, and this rate increases significantly with age, especially among those aged 70–80+ years.2 Prevalence is higher in females (4.8%) compared to males (3.4%), and age is a strong predictor, with older cohorts much more likely to have had knee replacement surgery.2 Many patients with knee osteoarthritis will eventually undergo TKR during their lifetime, reflecting both the high burden of osteoarthritis and the effectiveness of the procedure in restoring mobility and reducing pain.
PT plays a crucial role both before and after surgery. Preoperative “prehab” can help improve physical function and shorten hospital length of stay, preparing patients with better baseline strength and joint flexibility. Postoperatively, structured PT is essential to restore knee ROM, reduce pain, improve muscle control and support a return to daily activities and long-term mobility, making it a cornerstone of successful total knee replacement recovery.
The most common reason for total knee replacement surgery is arthritis, particularly osteoarthritis, which causes progressive cartilage breakdown, joint space narrowing, pain, stiffness, and loss of function. Osteoarthritis is a degenerative condition that worsens over time and is the leading indication for knee replacement when conservative treatments no longer provide adequate relief.3
Rheumatoid arthritis and other inflammatory forms of arthritis can also lead to the need for TKR. These autoimmune conditions cause chronic inflammation of the joint lining, resulting in cartilage damage, joint deformity, and persistent pain that may significantly impair mobility and quality of life.4
In addition to arthritis, knee trauma is a common contributor to knee joint degeneration. Prior injuries such as fractures, ligament tears, or meniscus damage can alter joint mechanics and accelerate cartilage wear, leading to post-traumatic arthritis. Over time, this damage may progress to severe pain and functional limitations that make total knee replacement the most effective treatment option.4
Understanding the underlying cause of knee damage helps guide both surgical decision-making and postoperative rehabilitation, allowing PT to be tailored to each patient’s specific need and long-term functional goals.

Preparing for a total knee replacement begins before surgery, and PT plays an important role during this phase. Preoperative PT focuses on improving knee strength, flexibility, and overall mobility, which can help patients better tolerate surgery and support smoother postoperative recovery.3 Preoperative exercises often target the quadriceps, hamstrings, hips, and core to promote joint stability and improve functional movement patterns prior to the surgery.3
PT begins within the first 24 hours post surgery and plays a critical role in the early recovery phase. During this time, physical therapists (PTs) focus on restoring safe mobility, protecting the surgical knee, and preventing postoperative complications such as stiffness, weakness, blood clots and delayed functional recovery.3
Early PT interventions typically include gentle ROM exercises to promote knee flexion and extension, quadriceps activation exercises to address postoperative muscle inhibition, and bed mobility and transfer training to help patients safely move in and out of bed or chairs. PTs also initiate gait training, often using assistive devices such as walkers or crutches, to encourage proper walking mechanics and reduce fall risk.3
Pain and swelling management are key components of immediate post operative PT. Therapists use movement-based strategies, positioning, and education to support circulation, reduce edema, and improve comfort while encouraging safe activity progression. Patients are also educated on proper limb positioning, activity pacing, and the importance of early movement to support healing and functional recovery.
Throughout this early phase, a personalized treatment plan is essential. PTs continuously assess pain levels, swelling, strength, mobility, and functional tolerance to guide exercise progression and activity recommendations. This individualized approach helps ensure safe recovery, supports independence, and sets the foundation for long-term strength, mobility, and successful outcomes.2
Seeking professional guidance throughout both the pre- and post-operative phases helps optimize outcomes following TKR. With consistent PT and individualized care, patients can improve confidence in movement, support long-term joint health, and return to meaningful daily activities with greater ease.
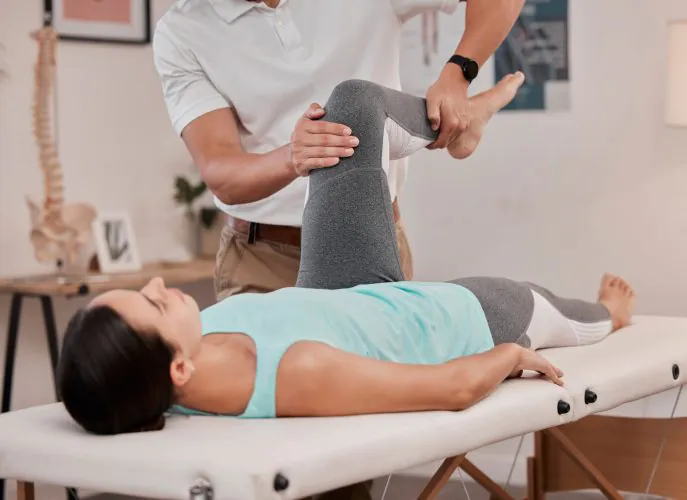
PT is essential for effective recovery following total knee replacement, guiding patients through a structured and progressive rehabilitation process that restores movement, function, and confidence. PTs begin with a comprehensive initial assessment, evaluating pain, swelling, ROM, strength, gait, functional mobility, and individualized goals. At Confluent Health, this assessment is used to develop a personalized treatment plan that prioritizes safe progression, functional independence and long-term joint health.
Improving mobility is typically the top priority early in rehabilitation, regaining full knee extension and flexion is emphasized before progressing too far into strengthening, as adequate ROM is essential for walking, stair climbing, sitting and standing, and most ADLs. Early restoration of knee motion is associated with improved functional outcomes and reduced risk of postoperative stiffness.2
PTs introduce targeted mobility exercises to safely improve knee joint motion, including active and assisted ROM exercises, gentle stretching, and functional movements that reinforce proper joint mechanics. These interventions are carefully progressed based on healing stage, swelling, and patient tolerance to support safe and effective recovery.3
As mobility improves, physical therapists provide ongoing education and movement guidance to help patients regain confidence with walking and daily activities. Instruction on gait mechanics, activity pacing, and movement strategies supports independence while minimizing setbacks. By prioritizing mobility first and layering in strengthening at the appropriate time, PT helps patients achieve meaningful functional improvements and supports a successful recovery.
Once adequate knee mobility is restored, PT shifts towards progressive strengthening to support joint stability, improve functional movement, and protect the new knee during daily activities. Strengthening focuses on the muscles surround the knee joint–particularly the quadriceps, hamstrings, gluteal muscles, and calf muscles–as these muscle groups are essential for walking, stair negotiation, transfers, and balance.3
PTs introduce targeted strengthening exercises that are appropriate for each stage of recovery. Early exercises may include quadricep sets, straight leg raises, seated knee extensions, and supported standing exercises to re-establish muscle activation while minimizing joint stress. As strength and tolerance improve, therapy progresses to closed-chain exercises such as sit-to-stands, step-ups, partial squats, and functional balance activities that better simulate real world movements.5
A progressive strengthening plan is critical to safe and effective recovery after TKR. PTs carefully advance resistance, repetitions, and functional demand based on swelling, pain levels, movement quality, and individual goals. This gradual progression helps rebuild strength without overloading healing tissues, reducing the risk of setbacks while supporting long-term functional outcomes.2
By addressing strength deficits through a structured and individualized program. PT helps patients regain confidence in movement, improve endurance and return to meaningful activities. Consistent strengthening guided by a PT plays a key role in maximizing outcomes and supporting long-term success after total knee replacement surgery.
Balance and stability training are essential components of PT following TKR, as surgery can temporarily disrupt proprioception, muscle coordination, and postural control. Weakness, pain, swelling, and altered movement patterns can increase the risk of instability, making targeted balance exercise critical for safe mobility and long-term recovery.6
PTs incorporate progressive balance and stability exercises to retain the body’s ability to sense joint position and respond to movement demands. Early interventions may conclude weight-shifting activities, supported single-leg stance, and controlled gait training, As patients progress, therapy advances to dynamic balance exercises, uneven surface training, and functional tasks such as turning, stair navigation, and transition; movements to improve real-world stability.7
Targeted balance training plays a key role in reducing all risk and postoperative complications. Research shows that balance-focused rehabilitation after knee replacement improves functional outcomes, walking, confidence, and overall safety during ADLs.8 PTs continuously assess movement quality and adapt exercises to ensure appropriate challenge without compromising joint integrity.
By emphasizing balance and stability alongside mobility and strength, PT helps patients move with greater confidence and control. This comprehensive approach supports safer recovery, promotes independence, and reduces the likelihood of falls as patients return to higher levels of activity following TKR surgery.
Pain management is a key focus of PT following total knee repealment, especially during the early and middle phases of rehabilitation. Rather than masking symptoms, PT addresses the underlying contributors to pain–such as swelling, stiffness, muscle weakness, and altered movement patterns-to support meaningful and lasting recovery.
PTs use a variety of non-pharmocological pain management strategies to help patients move more comfortably and confidently. These may include therapeutic exercise, manual therapy techniques, guided movement retraining, swelling management strategies, activity modification, and education on pacing and positioning. Research supports the use of exercise-based rehabilitation to reduce pain while improving function after knee replacement surgery.7
The goals of PT sessions extend beyond pain reduction alone. Each session is designed to improve mobility, strength, balance, and functional independence while keeping pain at a manageable level. PTs continually adjust treatment intensity based on patient response, healing stage and individual tolerance to promote steady progress without exacerbating symptoms.
A personalized treatment plan is essential for effective pain management, as recovery experiences vary widely between individuals. By tailoring exercises and interventions to each patient’s needs and goals, PTs help reduce setbacks and support long-term success. This collaborative patient-therapist partnership empowers patients to take an active role in their recovery, improves confidence in movement, and leads to better overall outcomes.
Patients experiencing ongoing or limiting pain are encouraged to take proactive steps toward seeking PT. Early intervention and consistent guidance can help manage discomfort, improve recovery efficiency, and restore quality of life after knee replacement surgery.
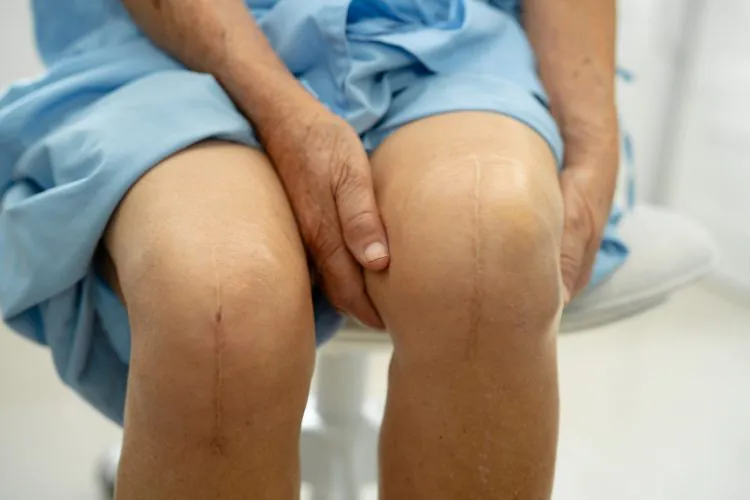
If you’ve recently had a TKR–or are preparing for surgery–taking proactive steps with PT can make a significant difference in your recovery. Early and consistent rehabilitation helps restore mobility, rebuild strength, improve balance, and reduce pain, setting the foundation for long-term function and independence.
Booking a consultation with Confluent Health allows our experienced PTs to assess your individual needs, design a personalized rehabilitation plan, and guide you safely through each stage of recovery. Don’t wait to take control of your healing–schedule your PT appointment today to start moving confidently and comfortably again.
PT is a critical part of recovering from a TKR, helping patients restore mobility, rebuild strength, improve balance, and manage pain. Every individual’s recovery journey is unique, and working with a skilled PT ensures a personalized plan that addresses your specific needs and goals. Seeking professional guidance early can optimize your outcomes and support a safe, confident return to daily activities.
PT typically begins within 24 hours after surgery. Early PT focuses on gentle mobility, safe transfers, and initial ROM exercises to reduce stiffness and prevent complications. Starting PT promptly helps accelerate recovery and supports long-term joint function.
Exercises start with gentle ROM and quadriceps activation to restore knee mobility. As recovery progresses, therapy includes strengthening, balance, and functional training to improve walking, stair climbing and daily activities. Your PT tailors exercise to your healing stage and individual goals for safe, effective rehabilitation.
Most patients participate in PT for 6-12 weeks, with frequency decreasing as strength, mobility, and independence improve. Patients should continue home exercise beyond formal PT sessions to maintain long-term function and reduce the risk of stiffness or weakness. Recovery timelines vary, and your therapist adjusts your plan based on your progress and goals.